It is time for healthcare mandatory training to evolve beyond completion-based models.
In complex healthcare systems, leaders rely on multiple forms of assurance to understand whether safety and quality are being maintained. Yet many organisations still rely heavily on a single indicator - training completion - as evidence that staff are prepared to deliver safe care. Completion, or participation rates, are useful, but on their own, tell us relatively little about what the workforce actually understands.
Increasingly, leaders are asking a different question of their training systems: how can I access more reliable insights into workforce knowledge and capability so I can make better, higher-value decisions?
This article explores how healthcare leaders can evolve their training systems, moving beyond traditional completion metrics as the only measure of the safety and quality of the care they provide.
Drawing on education, governance and high-reliability principles, this article explores knowledge verification as an approach that can help organisations make smarter decisions.
With a better understanding of how to deploy their training system, they can reduce unnecessary, low-value training burden for staff and L&D teams, gain reliable training data, and redirect finite resources and attention toward what matters most: supporting safe, respectful and person‑centred care.
The Traditional Model: Completion‑Based Training
For many years, mandatory training systems have operated on a simple premise: if a learner completes a training module, the requirement is met. Completion therefore becomes the primary metric reported to both internal and external stakeholders.
While this approach helps organisations demonstrate that training has been delivered, it provides limited insight into whether learners actually understand the material. Experienced staff may repeat content they already know, while leaders have little visibility into where genuine knowledge gaps and safety risks may exist.
In many organisations, this results in what clinicians sometimes describe as 'click‑through compliance'. This is where training requirements are technically satisfied, but the connection to learning and practice remains variable.
A Different Way of Looking at Training Assurance
Traditional completion metrics are like dashboard indicator lights. The light tells us that a process has occurred. A training module has been opened and completed.
But in complex care environments, leaders increasingly need more than confirmation that a process occurred. They need high reliability, confidence that the workforce understands the knowledge that underpins safe practice.
In this sense, completion is a signal. Understanding is the assurance.
Training systems that provide insight into workforce understanding therefore, offer a stronger form of assurance. One that aligns more closely with the expectations placed on healthcare organisations to maintain safe and capable workforces.
The Evolution of Mandatory Training
Traditional model: completion‑based training with limited insight into workforce understanding.
Transition model: knowledge verification introduces assessment of learning and identifies knowledge gaps.
Future model: capability‑based workforce development supported by data‑informed training systems.
A Transition: Introducing Knowledge Verification
Knowledge verification is an emerging approach in healthcare education. It introduces a structured, summative pre-assessment that is aligned to defined learning outcomes, allowing learners to demonstrate their existing knowledge, and only be required to repeat the training module if knowledge gaps are identified.
A summative assessment demonstrates that the learner has achieved the desired learning outcomes at a specific point in time. It demonstrates that the learner has sufficient understanding, which can give assurance that your staff have knowledge of a particular topic. If knowledge gaps are identified, the learner is redirected to the full training module.
This approach respects the knowledge and experience that healthcare professionals bring to their roles while ensuring that genuine knowledge gaps are addressed.
Knowledge Verification (KV) and the Workforce Capability Pathway
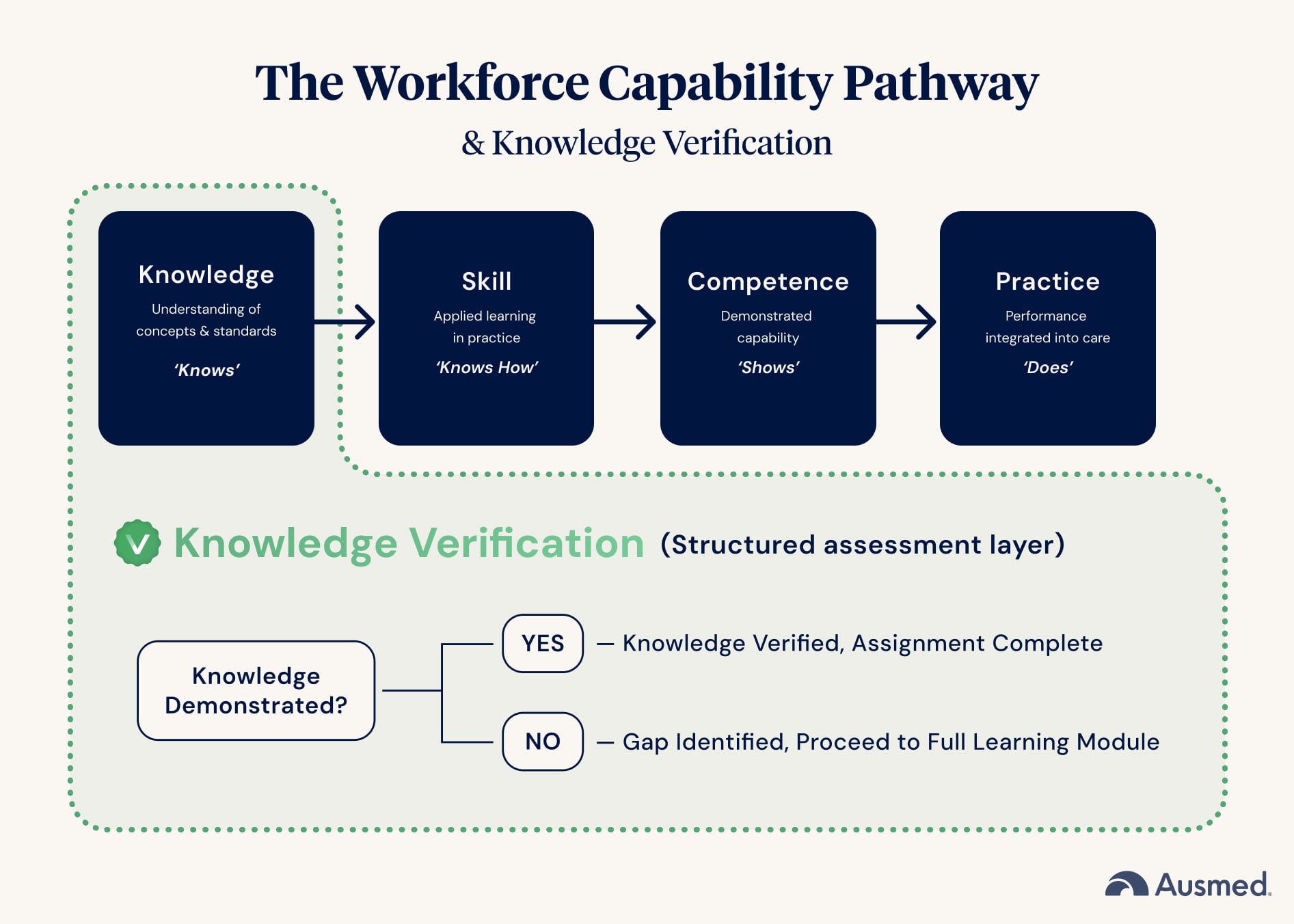
KV sits at the knowledge stage
It verifies understanding, not competence.
KV is a decision point
It determines whether learning is needed. If knowledge is demonstrated, the assignment can be entered as completed. If knowledge gaps exist, the learner proceeds to the full learning experience.
KV strengthens training systems
In verifying the learner's knowledge, the foundations of the capability pathway, you are strengthening, improving the reliability of your training system and related assurance metrics. It moves organisations from: Completion reporting → comprehension evidence.
Reclaiming Time for Care
An often-overlooked consequence of traditional mandatory training systems is the amount of time they require staff to spend away from the people they support.
In aged and acute care environments, time is one of the most limited resources. Every hour spent repeating low-value training that staff can demonstrate they understand is an hour that cannot be spent supporting residents, patients and families.
Approaches such as knowledge verification offer an opportunity to rebalance this. By allowing staff to demonstrate their understanding as a pre-assessment before repeating training, organisations can proactively reduce unnecessary training burden and ensure those who would benefit from training receive it.
This shift supports a care environment that is safe, respectful and person‑centred. It respects staff's experience, contributes to pride and engagement with their work, and fosters a sense that leadership are listening, which are attributes of a safety culture. It helps ensure that organisational attention is directed toward what matters most: supporting people receiving care and the teams who provide it.
From Completion Metrics to Comprehension Insight
Completion data can confirm that training occurred, but it cannot reveal what learners understood.
Introducing structured knowledge assessment allows organisations to move toward comprehension insights. Supporting decision makers in being able to reliably identify knowledge gaps, to more effectively target education, and to better understand whether training programs are strengthening workforce capability over time, and the relationship to organisational risk and performance.
Good governance underpins reliable, safe, Health systems.
Rather than a series of isolated training events, high‑reliability healthcare organisations increasingly view workforce development as a continuous micro-system, embedded and an enabler of the organisation's performance, risk and governance systems.
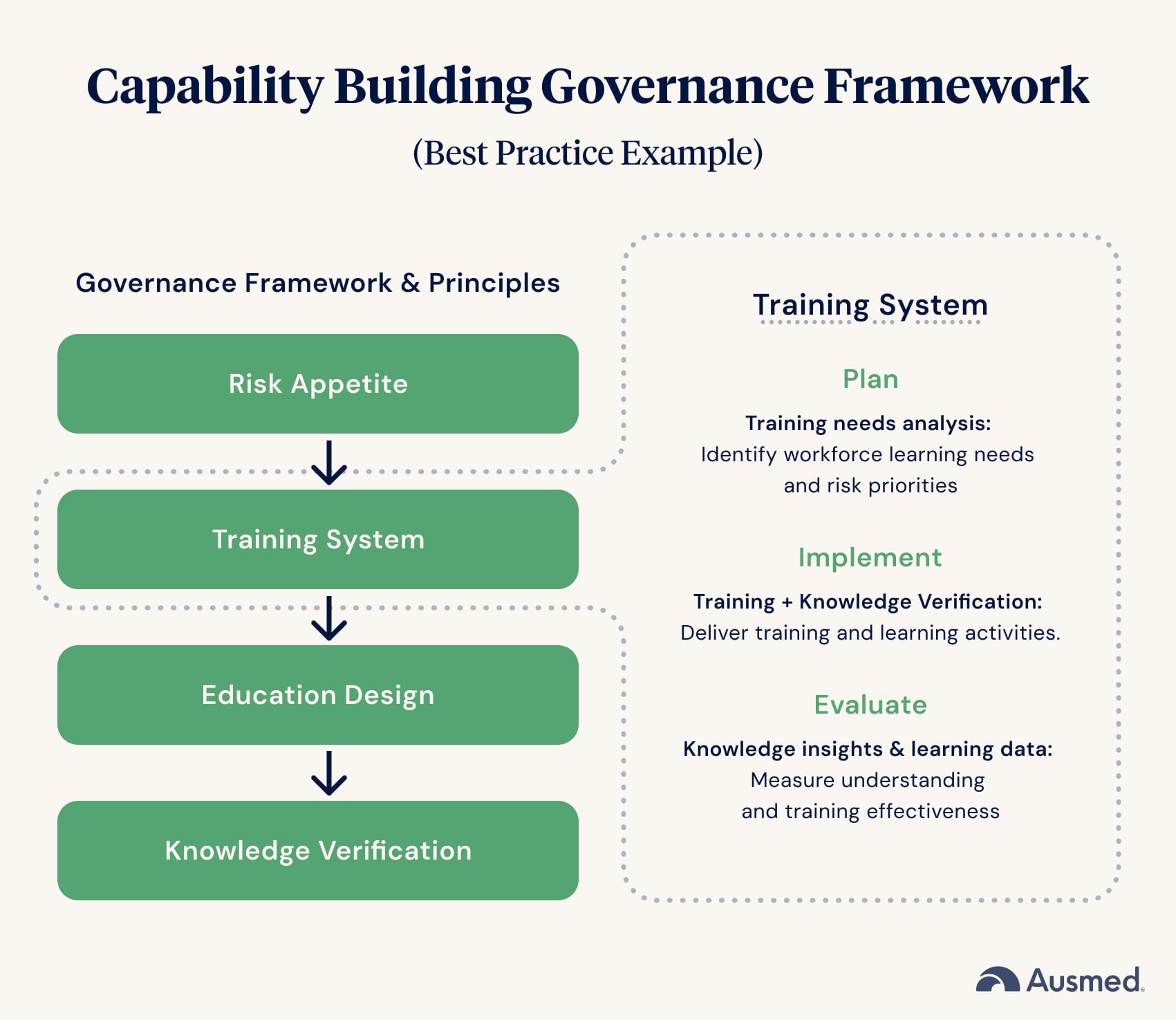
Leadership Opportunity
Changing established practices in healthcare is rarely simple. Mandatory training systems have developed over many years and are often shaped by regulation, organisational habit and understandable caution.
However, approaches such as knowledge verification provide leaders with something that has often been missing: clearer evidence of workforce understanding. With better evidence from improved evaluation data, organisations can critically review how they assure safe care environments rather than simply repeating processes because they have always been done that way.
This creates opportunities to redirect finite healthcare resources toward supporting staff in applying their knowledge in practice, developing skills, and strengthening healthcare teams.
Conclusion
Mandatory training has long been viewed as an administrative requirement within healthcare organisations. Yet the challenges associated with traditional models also create an opportunity for improvement.
If 'completion' is the dashboard light that signals a process has occurred, 'understanding' is the instrument that tells us whether the system is functioning safely.
Education systems that provide insight into a workforce's understanding therefore offer stronger assurance for leaders responsible for safety and quality.
As healthcare systems continue to evolve, organisations will increasingly need learning approaches that support capability, strengthen teams and allow staff to focus their time where it matters most: delivering safe, respectful and person‑centred care.





