What is a Stoma?
A stoma is a surgically created, artificial opening in the abdomen that allows waste (faeces or urine) to be diverted into a collection bag (Cancer Council 2021).
Common Types of Stomas
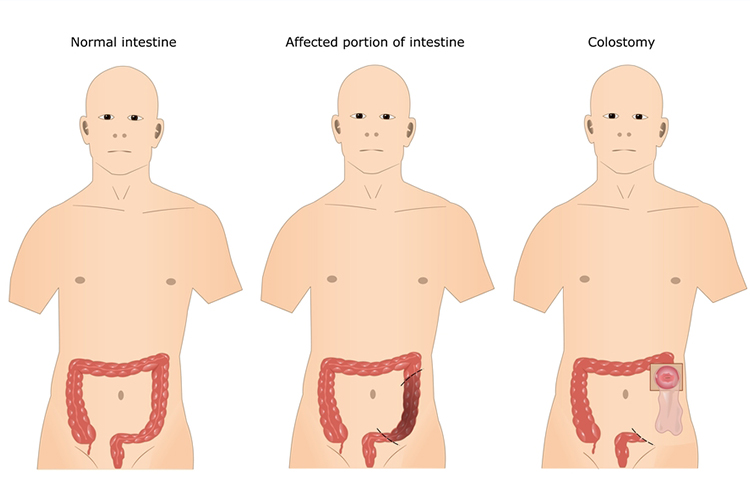
- Colostomy: A stoma created from the colon: an opening in the large bowel is made, and faecal flow is diverted.
- Ileostomy: Created from the ileum: an opening in the ileum (small bowel) is made, and faecal flow is diverted.
- Urostomy: A surgically-created diversion of urine: a urostomy may be necessary if the bladder is removed and the person needs an alternative way to pass urine.
(Cancer Council 2021)
The faecal matter collected by a stoma will vary depending on where in the intestines the stoma was created. An ileostomy can be expected to produce loose stools because it is closer to the small intestine, while a colostomy will produce soft and formed stools because it is near the rectum (Canadian Cancer Society n.d.).
The site also determines how active a stoma should be. An ileostomy appliance usually needs to be emptied four to six times a day, whereas a colostomy appliance will generally require emptying one to three times per day (Cancer Council Victoria 2021).
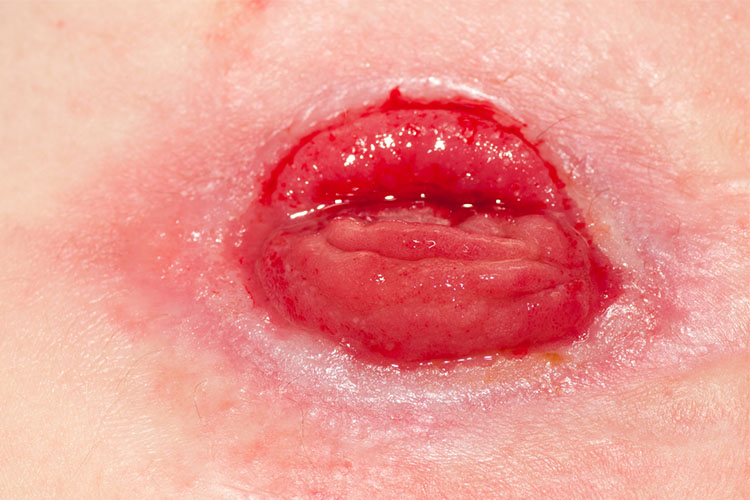
What is a Stoma Bag?
Waste that passes through the stoma is collected in a stoma bag, a pouch made from soft, waterproof material (CliniMed 2024).
This bag fits securely around the stoma and adheres to the abdomen using an attached or detachable flange. The type of bag needed will depend on the type of stoma (CliniMed 2024).
Reasons for the Formation of a Stoma
- Trauma induced to the abdomen
- Cancer in the bowel, bladder or pelvic organs
- Diseases such as diverticulitis, Crohn's disease or ulcerative colitis
- Congenital abnormalities
- Uncommon familial disorders
- Neurological disorders affecting toileting
- Degenerative changes in the bowel’s blood supply in preterm babies or older people
- After-effects of radiation therapy in the pelvic area.
(Healthdirect 2023; ACSA 2020)
How Long Does a Person Have a Stoma For?
A stoma can be permanent or temporary. Most stomas are temporary and reversed surgically after 3 to 12 months (Healthdirect 2023).
Psychological Impacts of Living with a Stoma
A stoma can be life-changing for an individual. Not only are they forced to come to terms with loss of control over their elimination of faeces or urine, but they may also experience other consequences such as changes to body image or psychosexual dysfunction, social isolation, stigma, embarrassment and decreased mood (McGrogan & Proctor 2024).
A study by Jayarajah et al. (2016) found that 16 to 26% of patients will experience negative psychological symptoms following a stoma creation immediately in the postoperative period. These symptoms are commonly anxiety and depression, but may also include suicidal ideation. Alarmingly, a year following their stoma creation, roughly the same percentage of people were still experiencing negative psychological symptoms.
Living Well With a Stoma
After a stoma operation, a person will need time to recover. This is normal, and the time needed will vary. The stoma will also undergo change in the first couple of weeks after surgery, in terms of both size and output (Coloplast 2021).
In general, a stoma should not prevent someone from working, socialising, exercising, travelling or other hobbies. A person’s physical and mental health will be important in determining their quality of life as they adjust to life with a stoma (Coloplast 2021).
Getting Used to a Stoma Bag
Having a stoma means that a person has no control over when they urinate or defecate. The stoma bag must always be worn to store the output (Coloplast 2024).
Healthy Skin
It’s important to keep the skin around the stoma clean and healthy so the stoma bag is able to attach properly. When the bag is attached in the correct way, there is no risk of smell and reduced risk of skin irritation. The patient should be educated on how to manage the bag and look after the skin around it (Coloplast 2021).
Food and Drink
For the most part, a person is able to eat and drink as they would usually. A person should monitor how their stoma reacts to certain foods. They should be advised if their stoma requires them to avoid or limit particular foods (Healthdirect 2023).
Sex and Intimacy
Following stoma surgery, it’s normal for a person to have concerns about the new appearance of their body, and it can take time to get used to these physical changes. Advise patients to talk to their partner about ways they could feel more comfortable during this transition (Coloplast 2021).
Talk About it
Approximately 50,000 Australians are living with a stoma (DoHaAC 2024). Remind the person they are not alone. It will likely help them to talk to someone about what they are going through.

Test Your Knowledge
Question 1 of 3
Approximately how many Australians are living with a stoma?
Topics
Further your knowledge
References
- Australian Council of Stoma Associations Inc. 2020, What is a Stoma, ACSA, viewed 11 February 2025, https://australianstoma.com.au/about-stoma/what-is-a-stoma/
- Canadian Cancer Society n.d., Colostomy and Ileostomy, Canadian Cancer Society, viewed 11 February 2025, https://cancer.ca/en/treatments/tests-and-procedures/colostomy-and-ileostomy
- Cancer Council 2021, What is a Stoma?, Cancer Council, viewed 11 February 2025, https://www.cancer.org.au/cancer-information/stoma
- Cancer Council Victoria 2021, Having a Stoma, Cancer Council Victoria, viewed 11 February 2025, https://www.cancervic.org.au/cancer-information/types-of-cancer/bowel_cancer/having-a-stoma.html
- CliniMed 2024, What is a Stoma Bag?, CliniMed, viewed 11 February 2025, https://www.clinimed.co.uk/stoma-care/stoma-types
- Coloplast 2021, Stoma Care After Surgery, Coloplast, viewed 11 February 2025, https://www.coloplast.com.au/ostomy/people-with-a-stoma/after-stoma-surgery/
- Coloplast 2024, Before Stoma Surgery, Coloplast, viewed 11 February 2025, https://www.coloplast.com.au/ostomy/people-with-a-stoma/before-stoma-surgery/
- Department of Health and Aged Care 2024, Stoma Appliance Scheme, Australian Government, viewed 11 February 2025, https://www.health.gov.au/our-work/stoma-appliance-scheme
- Healthdirect 2023, Living with a Stoma, Australian Government, viewed 11 February 2025, https://www.healthdirect.gov.au/living-with-a-stoma
- Jayarajah, U, Samarasekera, AM & Samarasekera D N 2016, ‘A Study of Postoperative Anxiety and Depression Among Patients with Intestinal Stomas’, Sri Lanka Journal of Surgery, vol. 34, no. 2, viewed 11 February 2025, https://sljs.sljol.info/articles/abstract/10.4038/sljs.v34i2.8261/
- McGrogan & Proctor 2024, ‘Survivor to Thriver: Identifying And Overcoming the Psychological Effects of a Stoma’, BJN, vol. 33, no. 16, viewed 11 February 2025, https://www.britishjournalofnursing.com/content/mental-health/survivor-to-thriver-identifying-and-overcoming-the-psychological-effects-of-a-stoma


