As a carer, it’s important to know what sensory loss is, how to recognise and differentiate it from expected age-related changes, and how to make adjustments for older people living with, or developing, sensory loss.
This article provides advice on supporting an older person experiencing sensory loss (specifically, loss of hearing, vision, taste, smell, and/or touch) to improve their safety, enjoyment and quality of life.
Sensory Loss Under the Strengthened Aged Care Quality Standards
Standard 5: Clinical Care - Outcome 5.5: Clinical Safety under the strengthened Aged Care Quality Standards (Action 5.5.10) requires older people with sensory impairment to be given access to and supported to use assistive devices and aids to improve their independence, function and quality of life (ACQSC 2024).
The Significance of Sensory Loss
Changes to hearing, vision, taste, smell and touch impact how a person experiences the world.
Sensory loss can impact:
- Communication
- Quality of life
- Daily living
- Enjoyment
- Socialisation, engagement and interaction
- Personal safety
- Independence
- Wellbeing
(MedlinePlus 2022; University of Chicago Medical Center 2016)
Sensory loss in older people is common. An American study found that 94% of older adults have one type of sensory loss; 38% have two; and 28% have three to five. These statistics are strongly associated with age, gender and race (University of Chicago Medical Center 2016).
In Australia, 93% of people over 65 years of age are experiencing a long-term vision disorder (AIHW 2021), and 50% of people aged 60-70 have some kind of hearing loss - this increases to 80% after 80 years of age (DoHaAC 2024).
Underlying factors of sensory loss in older people include nerve degeneration, environmental insults, genetic susceptibility, or a combination of these (University of Chicago Medical Center 2016).
Types of Sensory Loss
Hearing loss:
- The term ‘deafness’ encompasses a range of hearing loss, from partial loss of hearing to complete inability to hear.
- Causes include age-related hearing loss (presbycusis), exposure to noise, trauma, untreated ear conditions and hereditary or genetic disorders.
(Healthy WA 2018; DoHaAC 2024)
Vision loss:
- A person is legally blind if they can’t see at 6 metres what someone with normal vision can see at 60 metres or if their field of vision is less than 20 degrees in diameter.
- Causes include age-related macular degeneration, glaucoma, cataracts and diabetic retinopathy.
(Vision Australia 2023, 2024)
Oral loss - ‘Anosmia’ (smell/taste)
- As a person ages their smell sensitivity reduces. A loss of smell implicates the ability to taste.
- Causes include side effects of smoking, nasal mucus and adaptation (olfactory cells becoming flooded).
(Better Health Channel 2014)
Loss of touch
- As a person ages, reduced or changed sensations result.
- This may be an effect of decreased blood flow to the nerve endings or to the spinal cord or brain. It can be affected by brain surgery or nerve damage from chronic disease such as diabetes.
(MedlinePlus 2022)
Dual sensory loss
- Dual sensory loss, also known as ‘deafblindness’, is the impairment of both hearing and sight.
- About 100,000 Australians have deafblindness, two-thirds of these being older people over 75 years of age.
(Senses Australia 2021)
How to Care for and Communicate with Someone Who Has Hearing Loss
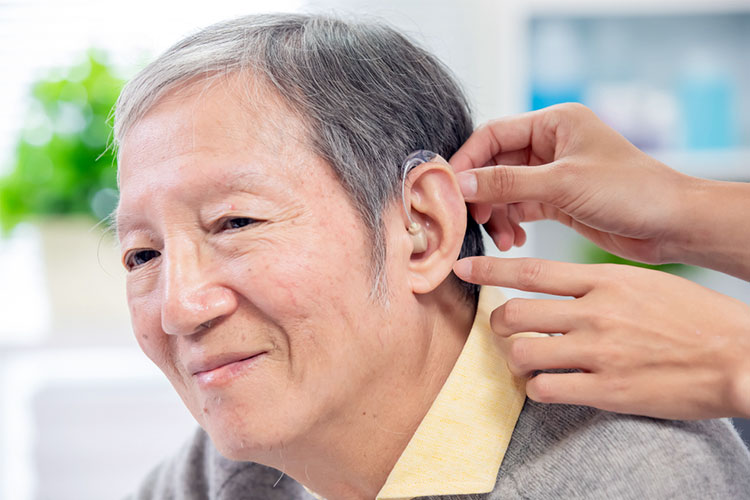
If a person in your care is over the age of 65, they should have their hearing tested every year (My Aged Care 2024).
As an individual:
- Stand in front of them when you’re speaking to them, and avoid speaking from another room.
- Say the person’s name before you start talking to them, giving them a chance to focus before you begin.
- Speak to the person with hearing difficulties rather than their interpreter (if they have one).
- Speak slowly and carefully without over-emphasising or distorting your lip movements.
- Raise your voice if necessary, but avoid shouting.
- Utilise body language and facial expressions when you speak, providing context.
- Consider writing messages if reading is less of a challenge for the person.
- Certain phrases may be harder to hear, so if a person is having trouble understanding you, try devising a different way of saying something.
- Remember that facial hair, eating or chewing and having your hands in front of your face will make it more difficult for the person to understand you.
- Reduce additional environmental noise.
- Ensure that hearing aids are functional and checked regularly.
- Reduce other distractions that may be present in the room.
(My Aged Care 2024)
As a facility:
- Install (and regularly check) visual smoke detectors.
- Investigate whether visual alerts such as alarm clocks and front door alerts may benefit the person.
- Install assistive listening devices to enable the person to contact help in an emergency.
(My Aged Care 2024)
How to Care for and Communicate With Someone Who Has Vision Loss

A person’s chance of developing a visual impairment rises significantly after the age of 40 (My Aged Care 2024).
- State your name clearly as you arrive.
- Use a neutral voice when speaking.
- Use everyday language - don’t avoid words such as ‘look’ and ‘see’ because you fear offending the person.
- Continue to use body language, as it can affect your tone of voice.
- If you are moving around a room or are about to leave, make sure to let the person know.
- Help or instruct a person when eating, for example, let them know where food is placed on their plate and its temperature.
- If you move something in a person's room, make sure to let them know.
- Be mindful of tripping hazards such as cords, wet floors, mops and buckets.
- Be aware that a half-open door is a hazard; keep doors either open or shut.
- If a person requests your assistance in walking, let them take your arm and then guide them by walking slowly while removing or describing obstacles in their path.
(My Aged Care 2024; Vision Australia 2022b)
How to Care for Someone Who Has Oral Sense Loss

With age, a person’s taste buds decrease in number and shrink, and their sensitivity to smell and taste diminishes (MedlinePlus 2022).
This not only impairs the enjoyment of eating but can also reduce the person's ability to sense certain dangers (e.g. being unable to smell smoke from a fire) (MedlinePlus 2022).
- Review the person’s medicines to determine whether any medicines are affecting their smell and taste and adjust if appropriate.
- Use different spices or flavours during food preparation.
- Implement safety devices (e.g. gas detectors).
(MedlinePlus 2022)
How to Care for Someone with Loss of Touch
The cause of a loss of touch as a person ages is likely the combination of a general loss of sensory acuity and comorbid conditions such as arthritis and cerebrovascular disease (Wickremaratchi & Llewelyn 2006).
A reduced sense of touch or feeling makes it difficult for older people to detect temperature, pain, vibration, pressure and/or texture. Talk to them about how you can make them more comfortable (Wickremaratchi & Llewelyn 2006; MedlinePlus 2022).
How to Care for and Communicate with Someone Who Has Deafblindness

Communication preferences for people living with deafblindness depend upon the extent to which the person’s vision and/or hearing are affected (Deafblind Information Australia 2021).
Consider the following modes of communication:
- Lip-reading
- Auslan
- Co-active signing: respectfully moulding a person’s hands to make signs
- Tactile signing: placing your hand over the hand of the signer to feel or read the signs
- Visual field signing: signing within the confined area of their vision
- Braille
- Printing on their palm
- The use of communication devices
(Deafblind Information Australia 2021)
Test Your Knowledge
Question 1 of 3
Complete the sentence: If a person in your care is over the age of 65, they should have their hearing tested ...
Topics
Further your knowledge
 Free
Free Free
FreeReferences
References
- Aged Care Quality and Safety Commission 2024, Standard 5: Clinical Care, Australian Government, viewed 23 May 2024, https://www.health.gov.au/resources/publications/strengthened-aged-care-quality-standards-august-2025?language=en/environment
- Australian Institute of Health and Welfare 2021, Eye Health, Australian Government, viewed 23 May 2024, https://www.aihw.gov.au/reports/eye-health/eye-health/contents/about
- Better Health Channel 2014, Anosmia - Loss of Smell, Victoria State Government, viewed 23 May 2024, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/anosmia-loss-of-smell
- Deafblind Information Australia 2021, Deafblind Communication, Deafblind Information Australia, viewed 23 May 2024, https://www.deafblindinformation.org.au/living-with-deafblindness/deafblind-communication/
- Department of Health and Aged Care 2024, About Ear Health, Australian Government, viewed 23 May 2024, https://www.health.gov.au/topics/ear-health/about
- Healthy WA 2018, Deafness, Government of Western Australia, viewed 23 May 2024, https://www.healthywa.wa.gov.au/Articles/A_E/Deafness
- MedlinePlus 2022, Aging Changes in the Senses, U.S. Department of Health and Human Services, viewed 23 May 2024, https://medlineplus.gov/ency/article/004013.htm
- My Aged Care 2024, Caring for Someone With Hearing, Vision and Oral Health Difficulties, Australian Government, viewed 23 May 2024, https://www.myagedcare.gov.au/caring-someone-hearing-vision-oral-health-difficulties
- Senses Australia 2021, Seen and Heard, Senses Australia, viewed 23 May 2024, https://www.deafblindinformation.org.au/wp-content/uploads/2021/01/SEN5964_Ending_the_Isolation_Resource_A4_WEB-Spreads_V3.pdf
- University of Chicago Medical Center 2016, ‘Sensory Loss Affects 94 Percent of Older Adults’, ScienceDaily, 18 February, viewed 23 May 2024, https://www.sciencedaily.com/releases/2016/02/160218083221.htm
- Vision Australia 2023, How do You Know if You Have Low Vision?, Vision Australia, viewed 23 May 2024, https://www.visionaustralia.org/services/eye-conditions/low-vision
- Vision Australia 2022, Tips on Communicating to Patients with Vision Loss, Vision Australia, viewed 23 May 2024, https://www.visionaustralia.org/news/tips-communicating-patients-vision-loss
- Vision Australia 2024, Understanding Eye Conditions, Vision Australia, viewed 23 May 2024, https://www.visionaustralia.org/services/eye-conditions
- Wickremaratchi, MM & Llewelyn, JG 2006, 'Effects of Ageing on Touch', Postgraduate Medical Journal, vol. 82, no. 967, pp. 301-4, viewed 23 May 2024, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2563781/

